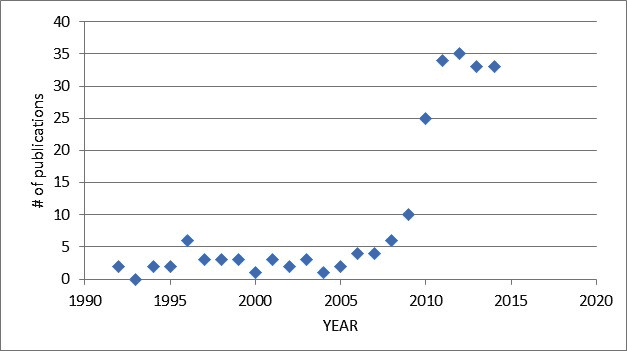
To begin, a graphical presentation of the publications (PUBMED) over the years (revised December 11, 2014)
During the past year, 17 scientific publications, 3 case reports, 6 editorials, and 8 reviews were published, for a total of 33 papers on PubMed.
ADULT studies:
1. NAVA vs. PAV vs. PSV in difficult to wean patients
In seventeen difficult to wean adult patients, Akoumianaki et al. (Respir Physiol & Neurobiology) compared physiologic parameters (Edi, Pes, Pdi, breathing pattern and arterial blood gases) during two 20-min periods of NAVA or PAV or PSV, without or with a respiratory challenge (added dead space or added load). The assist levels were set to obtain matching Pdi. Compared to PSV, both NAVA and PAV demonstrated proportionality between effort and VT, as well as improved variability in tidal volume. Trigger delays were significantly longer during PAV and PSV compared to NAVA.
2. Patient-ventilator interaction in non-invasive ventilation (COPD)
In the study of Doorduin et al (Crit Care), twelve COPD patients were ventilated with non-invasive NAVA (NIV-NAVA), PSV with a dedicated NIV ventilator), and PSV with an ICU ventilator, for 20 min. Patient-ventilator interaction was evaluated with automated analysis method (NeuroSync index). The NeuroSync index was higher (more asynchrony and dys-synchrony) with the two PSV modes compared to NAVA. No differences in blood gas values or respiratory discomfort were found between modes.
3. Heart-lung interactions during NAVA
Berger et al (Crit Care) performed a study in 10 cardiac-impaired intubated patients (with and without COPD), and compared the effects of incremental PSV and incremental NAVA in right ventricular function (using Pes, echo, and pulmonary artery catheter). Three levels of NAVA and three levels of PSV were randomised, for 20 min each. The main finding was that during NAVA, an increase in right ventricular outflow impedance was avoided by the maintained negative deflections in intrathoracic pressure (Pes). During PSV, Pes deflections were positive (over-assist) and right ventricular outflow impedance was increased.
4. Neural Indices for predicting successful discontinuation of mechanical ventilation
In eighteen ready-to-be-weaned patients, Muttini et al (J Crit Care) recorded Edi, Vt, and respiratory rate during baseline NAVA settings, NAVA50%, and during CPAP (initially 15 min and if tolerated, an additional 30 min period). Success was defined for those who could tolerate 30 min of CPAP without signs of fatigue. Various neural indices were calculated, namely the “P/I index” (Edi peak divided by the area under the Edi curve, EdiAUC), the neuroventilatory efficiency (vt/Edi pk), neural inspiratory time, neural expiratory time, and the Edi duty cycle (Nti/Ntot), and the rapid shallow breathing index (rr/VT). Nine patients were classified as success, and were extubated within 1 day from the end of the study. In both the success and failure groups, Edipk and EdiAUC correlated, however, the slope – and therefore the P/I index – were higher for the failure group. The predictivity performance of the P/I index was higher than that of the RR/Vt index (and was independent of the level of assist).
5. Order of respiratory muscle recruitment during NAVA vs. PSV
An electromyographic study was performed in twelve ventilated patients by Cecchini et al (CCM) to determine the distribution of neural drive to the various inspiratory muscles during NAVA vs PSV at three different levels of assist. Edi, and the EMG of the scalenes (EAscal) and alae nasi (EAan) were simultaneously recorded, and their relative contribution to Edi were calculated. With increasing levels of assist, in both PSV and NAVA, the electrical activity of all the studied inspiratory muscles decreased. However, compared to PSV, during NAVA there was a more prominent contribution of the diaphragm to inspiratory effort.
6. Use of Edi waveform for assessing auto-PEEP during PSV and NAVA
From the same group, Bellani et al (CCM) aimed to assess whether or not the Edi waveform could be used to estimate auto-PEEP in patients ventilated with PSV or NAVA. In ten intubated patients suspected of having auto-PEEP, they measured Edi, esophageal pressure, volume and flow during different levels of externally applied PEEP (2-14 cm H2O). They analyzed the tracings for dynamic auto-PEEP (Pes deflection before start of flow), an Edi-equivalent (Edi value at start of flow), and the delay between onset of Edi and flow. They found that the pressure required to overcome auto-PEEP was less during NAVA, The edi at the onset of flow was lower, and the time delay between Edi and onset of flow was less, compared to PSV, at all levels of external PEEP.
7. Increasing NAVA vs. PSV in healthy subjects
In this healthy-subject physiological trial, Meric et al (Respir Physiol & Neurobiol), four levels of NAVA and PSV were provided to subjects randomly for at least 8 minutes to establish steady state breathing of at least 6 minutes. They used of optoelectric plethysmography (lung volume distribution), transcutaneous CO2, and Edi to show that, different from PSV, increasing NAVA levels did not change Vt or PtCO2, and concluded that these two parameters cannot be used to titrate the assist level.
8. Sedation reversal and impact on Edi in ARDS Roze et al (British J of Anesthesia) studied 13 patients with ARDS who had been heavily sedated and on controlled ventilation for more than 4 days. Flumanezil was given to awaken the patients, in order to evaluate neurological status. During this period, Edi recordings were performed before and after Flumanezil injection (5 min pre and 5 min post), as well as VT and respiratory rate, during pressure support ventilation. Flumanezil provoked a significant increase in Edi peak, VT and respiratory rate. The study emphasizes the use of Edi as a “sedation monitor”.
PEDIATRIC and NEONATAL Studies
9. Randomized trial of NAVA vs. standard ventilation in PICU
In this randomized controlled trial, 175 infants (65% post-op) received either NAVA (n=85) or conventional ventilation (n=85). The relevant clinical outcomes included sedation use, time on ventilation, PICU length of stay, peak inspiratory pressure. Sedation use was lower in the NAVA group when post-op patients were excluded (no difference between modes for the entire population). Lower peak inspiratory pressure and oxygen requirements were found for the NAVA grioup). Median time on the ventilator was nor different between groups. For those infants adhering to the protocol, there was a significantly lower time in PICU for the NAVA group.
10-11. Daily monitoring of Edi in pediatric ICU (2 studies)
In 2014, 2 large studies (one in Canada, one in Finland) were performed to evaluate the Edi over the course of PICU stay. Emeriaud et al (Intensive Care Medicine) studied 55 critically ill infants during the acute stage, during the pre-extubation period, during the post extubation period, and during the day of PICU discharge. Edi pk was markedly supressed (3.6 microvolts) during the acute stage (infants were on conventional ventilation), and increased to 4.8 microvolts in the pre-extubation phase. Periods of diaphragm inactivity were frequent during the acute phase, even with low levels of assist. Shortly after extubation, Edi pk increased to 15 microvolts, and remained at this level (12 microvolts at the day of discharge). Patients with lung pathology exhibited higher Edi pk. The authors concluded that the Edi is low in the acute phase and cautioned the use of over-assist and over sedation.
A second study, measured Edi pk in 81 patients undergoing NAVA ventilation in the PICU (Kallio et al, Pediatric Pulmonology) during the acute phase and during and an hour after extubation. Edi was targeted to 5-15 microvolts (by NAVA level adjustment). Patients with lung pathologies (n=15) had higher Edi pk than post-op patients (n=66) in all phases of treatment. Post extubation, infants with lung pathology demonstrated Edi pk values of 20 microvolts (compared to 9 microvolts in post-op).
12. Use of Edi monitoring during high-flow nasal cannula in bronchiolitis
Pham et al (Pediatric Pulmonology) used the Edi signal and esophageal pressure, in 14 infants with bronchiolitis and in 14 infants with cardiac illness, to study the impact of high flow nasal cannula on the work of breathing. Respiratory impedance tomography was used to assess end-expiratory lung volume. Babies were studied for 10 min during HFNC and for 10 min without assist. Edi peak was higher in infants with bronchiolitis, compared to infants with cardiac disease. Both groups showed a significant reduction in Edi pk compared to “no assist”, although the diaphragm deactivation was more pronounced in the bronchiolitis group.
13. NAVA vs. PRVC in preterm infants (12-hrs): respiratory rate and central apnea.
In 14 intubated preterm infants, Longhini et al (Neonatology) compared 12 hours of ventilation with PRVC to 12 hours of ventilation with NAVA, in a cross-over trial. The main findings of this study were clear differences between neural respiratory rate and ventilator respiratory rate: in PRVC, the ventilator rate was could be 5 times higher than the neural respiratory rate, indicating auto-triggering or backup ventilation. Central apnea was reduced with NAVA. Vt and peak pressures were less with NAVA.
14. Variability of breathing during NAVA and conventional ventilation in PICU
Considering that a reduction in breathing variability is associated with adverse outcomes, Baudin et al (Front in Pediatrics) retrospectively examined variability in Edi and ventilator pressure in 10 infants during NAVA, PSV, and PCV, using detailed analysis of variability. The patterns and variability were compared to 11 control (non-intubated infants, Edi only). Control infants had higher variability than mechanically ventilated infants. For the latter, NAVA demonstrated the greatest variability in Edi and pressure, compared to PSV and PCV.
15. Use of Edi monitoring during “Kangaroo Care” in preterm infants. Soukka et al (Early Human Development) are the first to report valid Edi measurements in preterm infants with and without Kangaroo Care (when an infant is positioned skin-to-skin with a parent, shown to improve hospital stay). Seventeen neonates were studied during NIV-NAVA (mean birth weight 900g, mean GA 28 weeks) while in the incubator, or during Kangaroo Care. Edi min values were lower during Kangaroo Care, with a tendency for lower Edi pk values, indicating less energy expenditure of the diaphragm.
16. Improved synchrony with NIV-NAVA in infants with bronchiolitis
In 11 infants with bronchiolitis failing nCPAP, NIV-NAVA or Pressure/assist control (PAC) with NIV were studied for 2 hours each in a cross-over design (Baudin et al, Pediatric Pulmonology). The asynchrony index was much higher in the NIV-PAC group (38%) compared to NIV NAVA (3%). Neural respiratory rate was similar during both modes, BUT ventilator rate was in error reporting lower rates during NIV-PAC.
EXPERIMENTAL/LAB studies
17. NIV-NAVA and lung protection in experimental model of ALI
In this animal study, Mirabella et al compared NIV-NAVA (with a single nasal prong, n=10) for 6 hours to controlled mechanical ventilation (n=10) delivered via endotracheal tube with a lung protective strategy. Markers of lung function and lung injury indicated superior lung protection with NIV-NAVA. There were no differences in vital signs, P/F ratio, and lung wet to dry ratio. In experimental acute lung injury, NIV-NAVA is as lung protective as VC 6 ml/kg with PEEP.

Can we have the presentatios at Nijmegen 2015,
Thank you,
C. Salas
Thank you this information is very exciting!